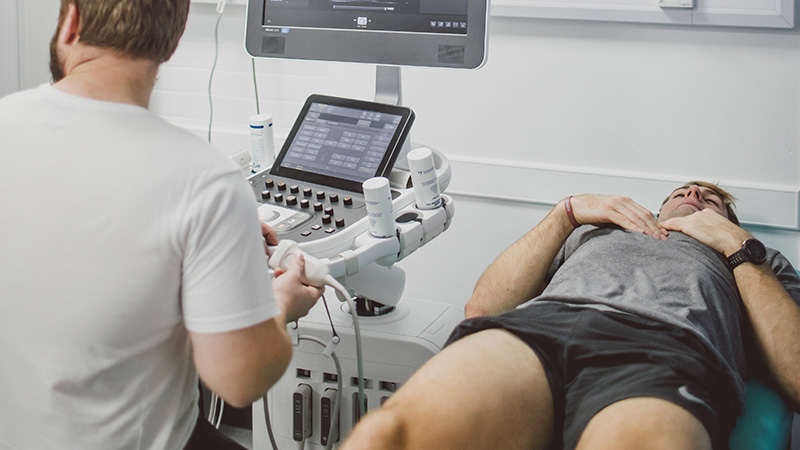
Our Physiotherapy, Occupational Therapy, Social Work and Sport Programmes offer a diverse range of placements for students in internationally renowned hospitals, community and industry settings. We are also proud to offer experience and placements in our Clinical Exercise and Rehabilitation (CLEAR) unit, our Health Clinics and our Activities of Daily Living (ADL) suite.
Our programmes examine contemporary issues related to sport, exercise, coaching and sports nutrition through theoretical, applied and professionalised methods of learning. The emphasis is on preparation for employability and development of high performing graduates, equipped with the skills they need to launch a successful career in their chosen field.